CHILDREN’S HOSPITAL
LOS ANGELES
A Comprehensive Quality Improvement Curriculum
“We aim to improve the health of our communities by working together to develop and implement quality measures that matter and make a significant difference in children’s lives.”
- CHLA Health Network Quality Mission
Background
The Children’s Hospital Los Angeles (CHLA) Health Network is a physician-led association connecting independent pediatric primary care practices in the LA region with the #1 ranked children’s hospital in the western U.S.
With a commitment to their patients and the Health Care Triple Aim, Health Network physicians actively participated in Learning Communities, a hybrid program that combined medical education with process improvement projects to achieve specific goals.
In its first two years, the program was rolled out to more than 20 pediatric practices with asthma, behavioral health, and well-child visits as areas of focus.
Triple Aim of Health Care
Researchgate.org
My Role
When I joined the Health Network, it was a newly formed venture with a medical director and CEO. With my experience in health care process improvement and human-centered approach, I focused on the development and implementation of quality improvement initiatives.
Led a team of four Health Network quality consultants + facilitated more than 50 workshops and trainings
Collaborated with subject matter experts on design and content of a curriculum tailored to the unique needs of our Health Network members
Designed the Learning Communities Workbook
Tracked and analyzed key performance metrics (KPIs) to measure the impact of these interventions
Improvement Goals
Asthma
Increase patient education + use of Asthma Action Plan, an individualized tool for patients to manage asthma
Behavioral Health
Expand capacity to screen, triage + manage depression, anxiety + ADHD in primary care settings
Well Checks
Increase well-child visit rates as a network per American Academy of Pediatrics schedule + guidelines
Learning Communities Success Story
“For the first time, I came home from a business trip and my son’s asthma was well controlled because my husband actually read and understood the asthma action plan.”
— Parent of asthma patient
Quality Improvement Program
Our Quality Program was designed to help Health Network physicians fulfill their American Academy of Pediatrics maintenance of certification criteria (MOC) through engaging and meaningful projects that would achieve measurable improvements in the services they provided to their patients.
The program design featured a synthesis of insights gathered from primary and secondary sources, including conversations with clinical experts and peer institutions working on similar initiatives to understand best practices and lessons learned.
Process improvement projects met certification requirements
My prior performance improvement experience informed program’s development
Clinical Microsystems framework was created at Dartmouth College
Target Audience
Our target audience consisted of independent pediatric practices scattered throughout LA county and beyond. To get to the root cause of problems, we felt it would be important to include all of the stakeholders, including nurses, clinical staff, and administrators and doctors. By incorporating these multiple points of view, we were more likely to expose inconsistent processes and call out assumptions + biases among team members.
Method
The Clinical Microsystems quality improvement method, pioneered at Dartmouth College, fit the needs of our target audience because it was designed for independent groups of health care coworkers (aka a microsystem) and smaller scale process improvement initiatives. The Clinical Microsystems framework was effectively aligned with the Health Network’s quality mission.
Clinical Microsystems Method
We used this step-by-step process, informed by Clinical Microsystems, in the development and roll out of our quality improvement projects and coursework.
Learning Communities Workbook
A Go-to Resource + Core Quality Coursework
I designed the Learning Community Workbook to address the needs of our target audience and contain comprehensive, clear, and meaningful content that would meet their maintenance of certification requirements. Each activity included directions and background content tied to Clinical Microsystems to enhance their learning experience.
It also served as a concise facilitator’s guide for quality consultants while facilitating trainings and workshops that would help support teams throughout the development and implementation of their process improvement projects from start to finish.
Learning Community Workbook
I partnered with marketing to design high-quality, CHLA-branded materials that were aligned with our Health Network quality mission.
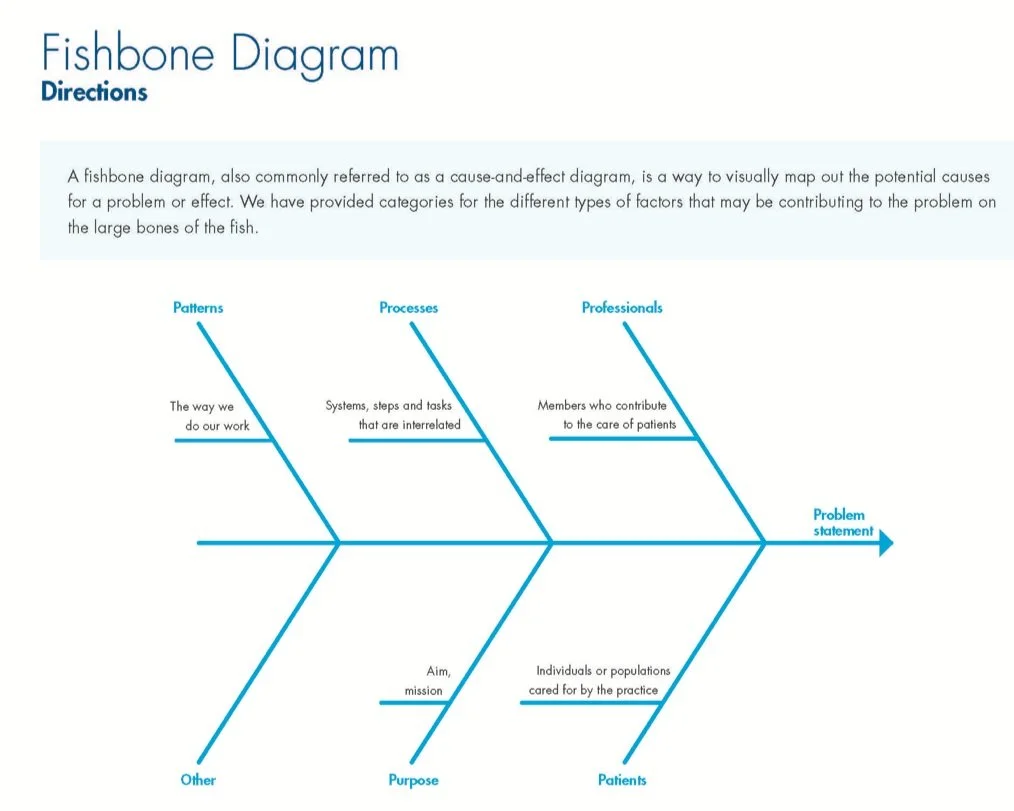
Fishbone Diagram
A page from the workbook used to generate ideas for potential causes and effects of a problem
Clinical Microsystems in Action
Step 1: Assessment
To kick off each practice’s quality improvement projects, we called upon all members of a practice to reflect and come to a consensus on core characteristics and values of their microsystem using the “5Ps” activity.
Sample 5Ps assessment outlines core characteristics and values of an independent practice
Step 2: Aim
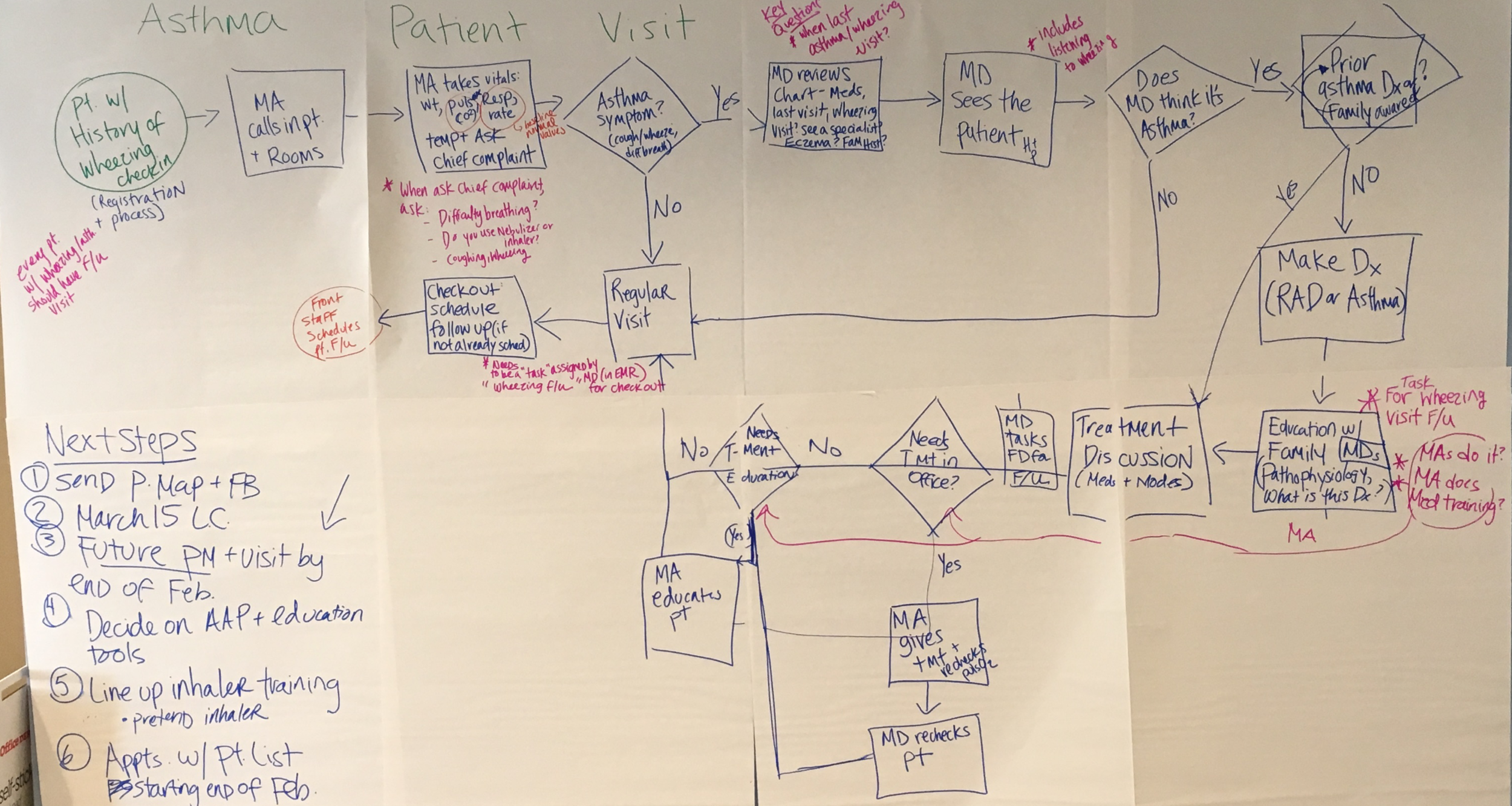
We elicited input from the entire practice team to construct a map of their current workflows and processes related to the area of focus i.e. an asthma visit.
This exercise revealed areas of delay, inefficiency, confusion, and inconsistency in daily processes and helped us pinpoint the areas for improvement.
An example of one practice’s current asthma visit workflow. Pink comments highlight areas of debate or confusion.
Step 3: Change Idea
Participants brainstormed potential causes of the problem and ideas for solutions/change ideas using a fishbone diagram.
Future Process Map: Once the change idea was chosen, we created a future process map that incorporated this new change in the process and served as a guide for all staff when carrying out the intervention. To keep each other accountable staff printed out copies and posted the map on the wall in common areas.
This fishbone diagram captures team brainstorm on potential causes of their practice’s low rate of completion of adolescent depression screenings.
Step 4: Implementation + Data
This final step represents the execution, tracking, and data collection of the practice’s change idea.
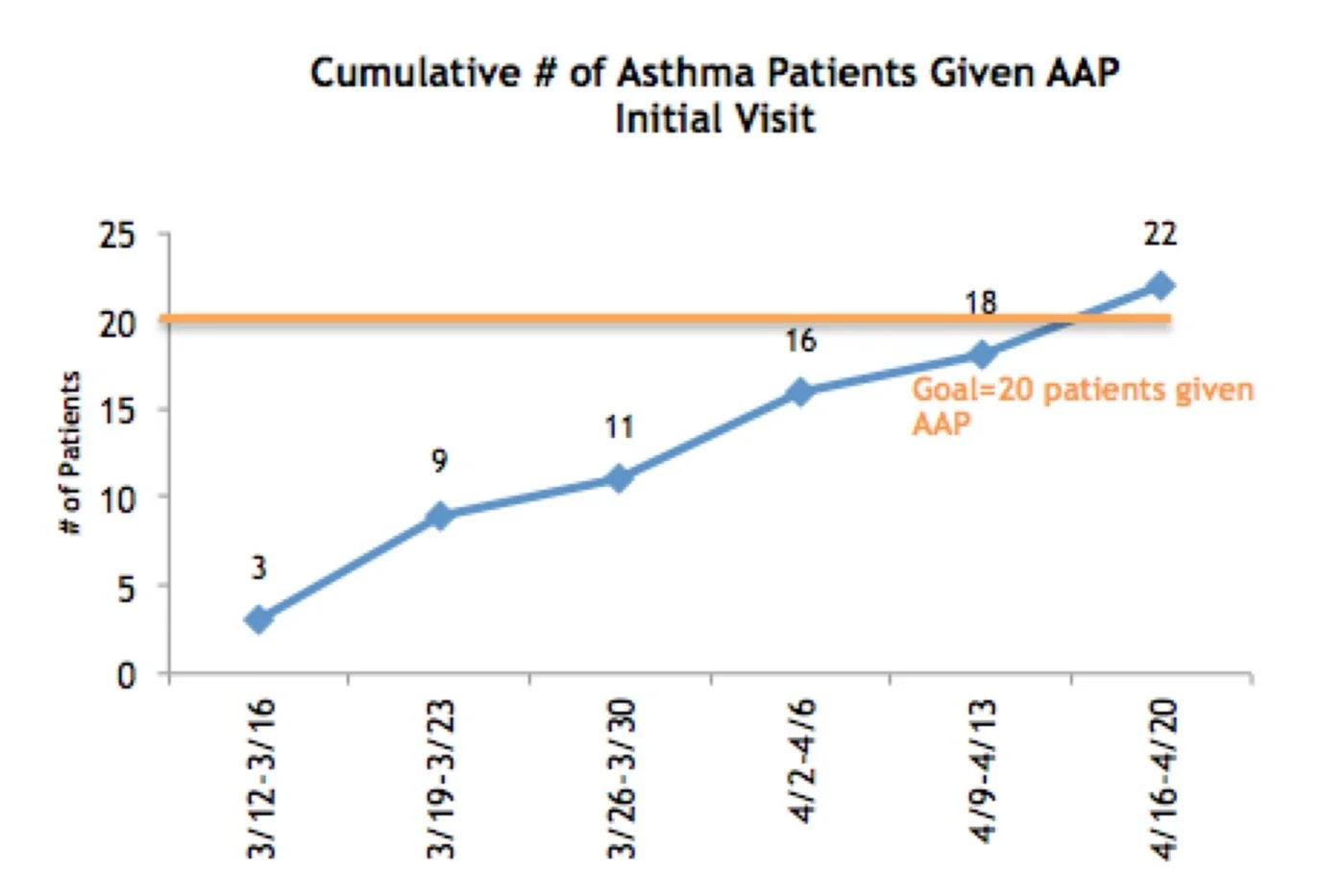
Aim: Achieve 60% Asthma Action Plan (AAP) completion rate
Change Idea: MD or PA provides AAP and asthma education to asthma patients at physical exam
Data Collection: Tracked AAP completion rates over 6 weeks
Result: Exceeded goal! 100% AAP completion rate
Sample practice data from the Asthma Learning Community
Key Challenge: Office Dynamics
At times we found it difficult to elicit input from certain staff members when their bosses were in the room.
Workflow exercises were designed to be a catalyst for honest conversations among team members about the pain points of their practice, but depending on the office culture and power dynamics, they could also make people feel uncomfortable.
In certain instances we held follow up conversations with smaller groups to build rapport and try to make people feel more at ease during the larger conversations.
Key Performance Indicators
How did we measure success?
To measure improvement we created a centralized dashboard of outcomes, process, and engagement measures that we tracked consistently across all of the practices.
These KPIs were determined in collaboration with data and clinical experts and prioritized based on clinical guidelines, feasibility, and institutional goals.
The hospital’s IT team helped us navigate certain data collection constraints, particularly because we were working off of different electronic medical records systems depending on each individual practice.
We collected data and checked in with practices regularly to assess their progress and made adjustments as needed to help them achieve success.
Key Metrics
-

We identified our key metrics by weighing our quality improvement priorities with our IT capabilities.
-

We provided staff with branded tools such as Asthma Action Plans to support interventions + track metrics.
-

Our KPIs included standardized health care benchmarks like PHQ-9 behavioral health screening rates.
First Year’s Results + KPIs Overview
800 patients impacted
38 physicians + 20 staff participated
38 workbooks completed
325 MOC credits granted
40 quality improvement trainings facilitated
672 emails/phone calls completed
22 process maps plotted
13 cause-effect diagrams mapped
20 clinical microsystems cycles completed
That’s me and my colleague with physicians and staff from a pediatric practice participating in the asthma learning community.
Medical Education
In addition to quality improvement projects, the Learning Communities medical education component provided opportunities for participants to learn foundational knowledge, the latest research findings, and best practices from experts and from each other through a series of lectures, e-learning, clinical trainings, and breakout sessions. Medical Education was led by CHLA faculty and prominent national experts on topics such as disease classifications, screenings, diagnoses, patient education, and treatment of complex conditions.
Medical Education Series
-

Clinical Training
Hospital staff and Health Network experts led trainings on current technology and tools for monitoring and treatment of patient conditions, including in-practice trainings.
-

Faculty Learning Collaboratives
CHLA faculty experts gave lectures + supported breakout sessions on relevant topics, including classification, treatment and patient compliance.
-

E-Learning
I adapted content to CHLA’s e-learning platform, which improved convenience + accessibility for far away practices.
Reflection
Working closely with individual practices, I had the opportunity to empathize with a variety of points of view - from the front end administrators to the most senior physicians. Playing the role of facilitator in this context was both challenging and exhilarating, particularly when we went through the process of unraveling the root causes of problems and inconsistencies with the ways they’ve been doing things as a practice.
Yet, one of the most gratifying aspects of the program went beyond witnessing improvements to processes and quality of patient care. The anecdotes and post-program feedback from participants indicated that the program made a deep impact on the emotional and professional growth of providers, including positive changes in their communications with patients and families.
One more note: While I’d argue that in-person connections between peers can never be fully replicated, our early decision to transition elements of the program to Webex and CHLA e-learning platform enhanced convenience (the drive to the hospital could take up to 3 hours for some participants!) and would later provide a more seamless transition to 100% virtual learning during COVID conditions.
Themes + Qualitative Feedback from Participants
Better communication with parents
“I learned great practical tips for how to talk to parents who are skeptical about vaccines - I loved hearing best practices from my peers.”
Increased empathy between doctors and families
“Patients were more capable of dealing with a chronic illness, which is always difficult and frightening for parents. I also think it increased their appreciation and respect for what we try to do as physicians.”
Enhanced understanding of complex conditions
I have a much clearer understanding of asthma classification - I’ve been under diagnosing my asthma patients.”
Greater confidence to confront issues that are often stigmatized or excluded from primary care visits
“It encourages me to have more proactive discussions with patients and consider prescribing for mood and anxiety disorders.”